Palliative care at home
Palliative care provides specialised support for people with life-limiting conditions. At Elder, we’ll match your loved one with the right carer, ensuring comfort, dignity, and care at home.

Used by 5,000+ families across Great Britain

More value
On average, services facilitated by Elder are 35% cheaper than traditional alternatives.
More control
Set your care hours from our custom built app. Manage and collaborate care with family.
More choice
View carer profiles, read reviews from other families, and arrange a video/phone call ahead of placement.
More support
From our family support specialist to our in-house clinical team, we’re on hand if you need us.

We are an award-winning marketplace connecting families and carers.
Every care story is personal, and ours is no different. Our founder, Pete, was inspired to help families like yours after struggling to find the right care for his own Gran, Frances. Fast forward to today and our platform has connected thousands of families and self-employed carers. Our tools personalise every care experience, eliminate unnecessary paperwork, and empower families to take control of later life.
What’s in this palliative care guide?
- What is palliative care?
- When should someone be offered palliative care?
- What conditions qualify for palliative care?
- What symptoms can be managed with palliative care?
- Why do doctors recommend palliative care?
- What can a live-in palliative carer do?
- How Elder can support with palliative care
- How to arrange live-in palliative care with Elder
- Palliative care vs hospice care: what’s the difference?
- Frequently Asked Questions
- Read more on palliative care
- Other types of care

What is palliative care?
Palliative care is specialised support for people with serious or life-limiting illnesses. Its primary goal is to improve quality of life by managing symptoms, alleviating pain, and providing emotional support to both the individual and their family.
Palliative care can be delivered at home, ensuring comfort and dignity while respecting the personal wishes of the patient. It is often provided in stages, depending on the progression of the illness — learn more in our guide to the 5 stages of palliative care.
When should someone be offered palliative care?
Palliative care should be offered when a person’s condition becomes difficult to manage with standard treatment alone, such as after a terminal diagnosis or during the progression of a chronic, life-limiting illness.
Palliative care may be offered early on to ease physical discomfort, reduce emotional strain, and provide tailored support. Whether care is needed for months or years, starting palliative support as soon as symptoms become challenging can make a difference to both the individual and their loved ones.
What else should be arranged alongside palliative care?

As part of planning for palliative care, there are two important legal and practical arrangements that can help ensure your wishes are followed and your future care is in trusted hands:
1. Advance Decision
This is a legal document that outlines your preferences for medical treatment and care in situations where you’re no longer able to communicate or make decisions yourself. It helps ensure your wishes are respected.
2. Lasting Power of Attorney
This is a trusted person you legally appoint to make decisions about your healthcare and personal affairs if you’re unable to do so. Choosing a Lasting Power of Attorney ensures someone can advocate for your best interests.
What conditions qualify for palliative care?
Palliative care is recommended for people living with a life-limiting or serious illness that cannot be cured but can be managed to improve quality of life.
Common conditions that may qualify for palliative care include:
- Advanced cancer
- Chronic lung disease
- Motor neurone disease
- Parkinson’s disease
- Dementia
- Advanced heart disease, such as congestive heart failure.
What symptoms can be managed with palliative care?
While many associate palliative care with pain relief, not everyone experiences pain the same way. In fact, symptoms can vary widely depending on the person, their diagnosis, and the treatment they’re receiving.
Some of the most common symptoms palliative care helps manage include:
- Pain – managed through medication and comfort strategies.
- Loss of appetite – often supported by small, frequent meals and tailored nutrition advice.
- Nausea – caused by treatment or illness, and eased with dietary changes or anti-sickness medication.
- Constipation – often due to medication or reduced mobility, supported with hydration and diet.
- Shortness of breath – eased by sitting up as much as possible, open windows or fans, and sometimes medication.
- Confusion – common in advanced stages of illness and addressed through medical care and environment adjustments.
- Difficulty sleeping – supported through routine, relaxation techniques, and, where appropriate, medication.
Palliative care teams tailor support based on individual needs, ensuring each person receives the right level of comfort, dignity, and care at home.

Why do doctors recommend palliative care?
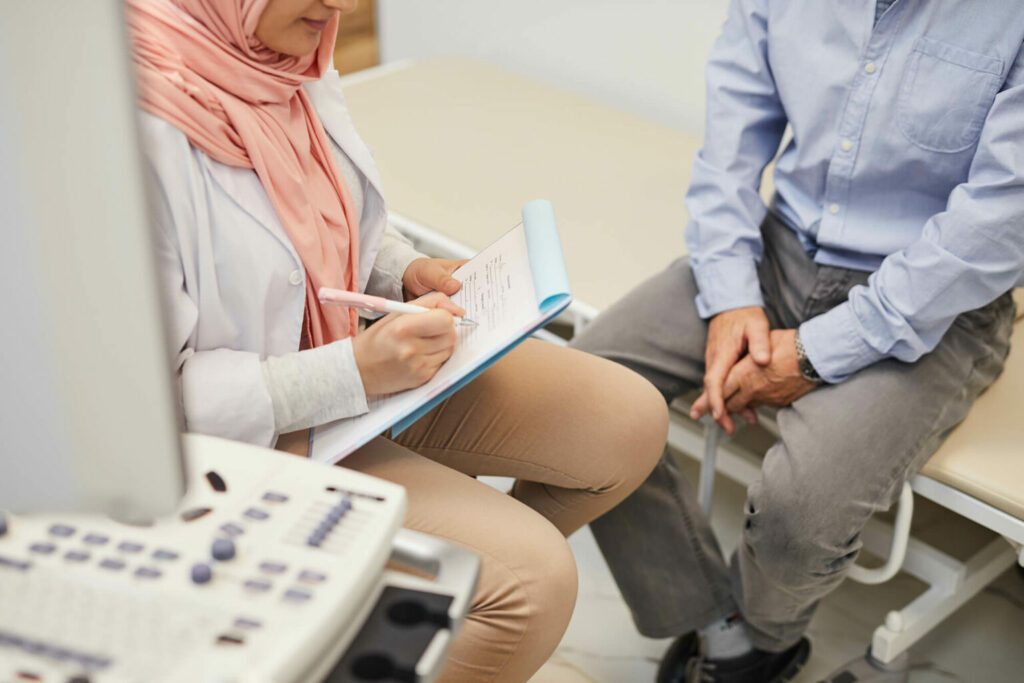
Doctors may recommend palliative care for a number of reasons, depending on the stage and nature of the illness. These can include:
- Following a diagnosis: Doctors may introduce palliative care after diagnosing a life-limiting condition to help patients and families plan ahead and understand their options.
- To support other treatments: Palliative care can run alongside treatments like radiotherapy, helping to manage symptoms and improve overall comfort.
- When a condition can’t be cured: If curative treatment is no longer effective, palliative care focuses on relieving symptoms and maintaining the best possible quality of life.
What can a live-in palliative carer do?
A live-in carer can become an essential member of your palliative care team – helping with symptom management and improving quality of life.
The professional carers in Elder’s network can assist with a wide range of tasks, including:

- Personal care – helping with washing, dressing, oral hygiene, and grooming
- Continence care – assistance with using the toilets or changing pads
- Family updates – sharing regular updates with loved ones who cannot be there every day
- Support for relatives – offering reassurance and emotional support to family members
- Daily routine – maintaining familiar routines to bring structure, comfort, and stability
- Therapeutic support – assisting with calming therapies like meditation or aromatherapy
- Household tasks – handling cleaning, laundry, pet care, and greeting regular visitors
- Meal preparation – planning and cooking nutritious meals that suit personal preferences
- Mobility support – helping move safely around the home to reduce falls and injuries
- Providing medication reminders – supporting with correct medication at the right times.
How Elder can support with palliative care
Live-in care can be a valuable form of palliative care, offering practical and emotional support to individuals and their families. It enables people to stay in the comfort of their own home as their condition progresses, rather than moving to a hospital, care home, or hospice – if that’s not needed or desired.
At Elder, our matching process helps you find a carer with the right skills, experience, and personality to meet your needs. This personalised approach ensures they can provide sensitive, one-to-one care while helping to maintain a sense of normality and routine.
Palliative care needs vary depending on the condition. For example:
- People with dementia may require long-term support as symptoms gradually progress.
- Those living with COPD often benefit from care after flare-ups or hospital stays.
- Older adults with cancer may need more intensive care over a shorter period, helping to relieve the burden on family and allow for more meaningful time together.
How to arrange live-in palliative care with Elder
1. Share your care request
Tell us your care requirements in our request form, including the type of care you’re looking for, any specialist skills you need, and what daily life looks like.
2. Select your carer
You’ll start receiving profiles of suitable self-employed carers within 24 hours. Chat to them online or arrange a phone or video call, before choosing who you like best.
3. Manage care
Once your agreement with your carer begins, use your MyElder account to chat with them and the Elder team, manage your schedule and care information, and find respite cover if you need it.
Palliative care vs hospice care: what’s the difference?
Palliative care and hospice care both focus on comfort, pain relief, and emotional support. The main difference is that palliative care can be given at any stage of a serious illness — often at home and alongside treatment — while hospice care is usually for those nearing the end of life and is often provided in a hospice setting.
| Live-in palliative care | Hospice care | |
|---|---|---|
| Stay in the comfort of home | ||
| Choice of meal times and food preferences | ||
| One-to-one, 24-hour support from a dedicated carer | ||
| Maintain usual routines and way of life | ||
| Friends and family can visit anytime |
FAQs about palliative care
Does palliative care mean death?
No, palliative care does not mean someone is dying. It’s a type of care that helps people manage the symptoms of serious or life-limiting illnesses at any stage. While it can include end-of-life care, many people receive palliative care for months or even years to improve comfort and quality of life.
How many forms of palliative care are there?
There are several forms of palliative care, each designed to address different aspects of a patient’s wellbeing. Common types include pain management, symptom control, emotional support, and spiritual care. These approaches work together to improve the quality of life for individuals with serious or life-limiting conditions.
Is palliative care free?
Palliative care can be free in certain situations. For example, hospice care, which supports end-of-life needs, is typically free and includes services like therapy and emotional support. You’ll usually need to be referred by a GP or nurse.
You may need to pay if you want additional home support for daily tasks unless you’re eligible for NHS Continuing Healthcare funding – this covers health and social care costs for those with significant care needs. Home adaptations for palliative care, such as ramps or grab rails, may also involve extra costs, but grants may be available to help.
For more information, read our guide to funding your care.
Who pays for palliative care at home in the UK?
In the UK, the NHS pays for palliative care at home as it is considered a primary health need. The local authority can carry out a needs assessment to determine the level of care and funding a person is eligible for.
How long does palliative care last?
Palliative care can last for as long as it’s needed. It can begin at any point after a diagnosis and may last for days, months, or even years.
Is there anything a palliative live-in carer can’t do?
When you choose a live-in carer through Elder, they will get to know your specific needs based on the information in your MyElder account. However, certain tasks require specialist training or fall under nursing care, and these are not typically covered by a live-in carer. These tasks include:
Administering pain relief or medication
STOMA care
PEG care
Wound care
Ventilation, Oxygen Support, BiPAP or CPAP Support
Unstable Epilepsy
Controlled Drug Administration
Glucose readings via finger pricks
Injections
Pessaries, Enemas, Suppositories
Caring for someone in active addiction.




