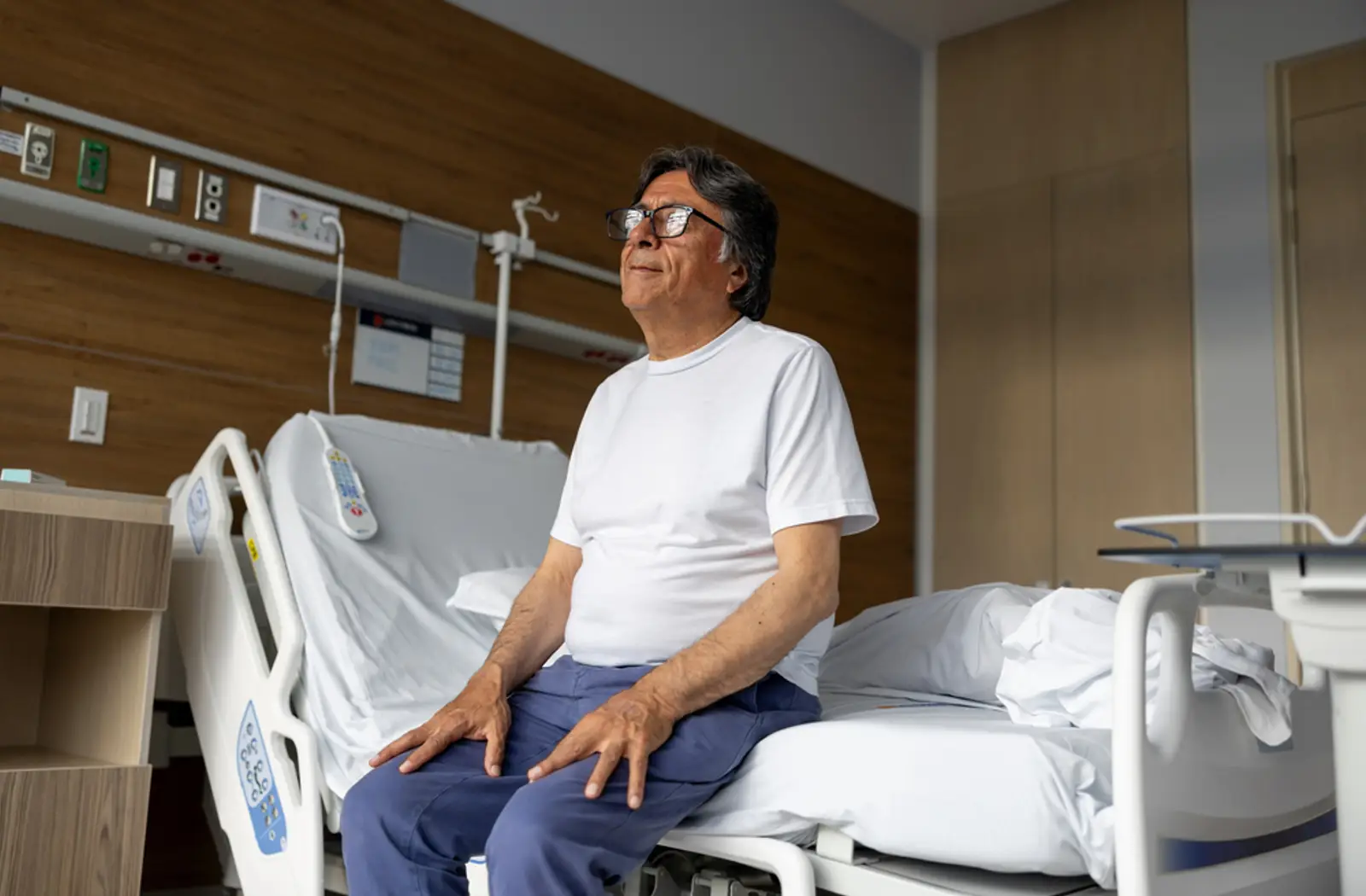
The 5 stages of palliative care
Palliative care provides medical, emotional, and practical support to people with a life-limiting illness through five key stages. At Elder, we’ll help you understand each step and arrange the right care.
Find a carerCall us

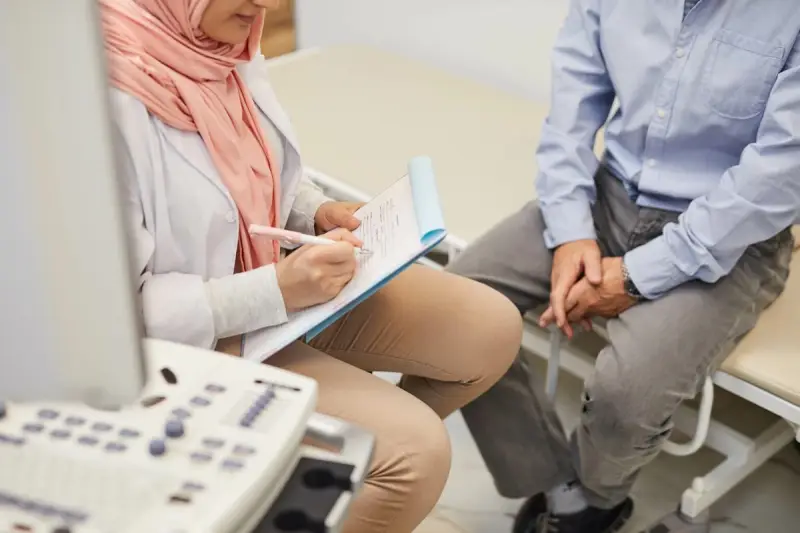
Palliative care explained
Palliative care is a type of support for people living with a life-limiting illness such as cancer, heart failure, or Alzheimer’s. It focuses on managing physical symptoms, easing emotional distress, and improving overall quality of life.
Palliative care can begin at the point of diagnosis and continue for months or years. It’s often delivered by a team of professionals who work together to support both the individual and their family.
For a fuller comparison of palliative care and end-of-life care, see our guide to the differences between end-of-life care vs palliative care.
What are the 5 stages of palliative care?
Stage 1: Creating a bespoke care plan
The first stage of palliative care involves creating a personalised care plan based on your diagnosis, current needs, and future preferences.
Questions to ask at stage 1:
- Who will be involved in my palliative care?
- Where will my palliative care take place?
- How long might I need support for?
Your GP, along with other healthcare professionals involved in your care, will help you identify the support you need now, and how it can adapt as your condition progresses.
This initial plan typically includes:
- Your current treatment and options for future care
- How your condition is likely to progress over time
- Medications and approaches for managing symptoms
- Your care preferences, such as staying at home or receiving a specific therapy.
You may also want to start thinking about future decisions, like setting up a Lasting Power of Attorney, creating an Advance Decision, or writing a living will. There’s no pressure to make these choices straight away, but it can help to begin the conversation early.
An Advance Decision outlines if and when you would want to refuse treatment or resuscitation, in case you’re unable to communicate your wishes later. It’s an important part of your care plan, and your doctor can help you understand what it means for your future care.

Stage 2: Providing emotional, spiritual and psychological support
The second palliative care stage is about emotional, psychological, and spiritual support — helping you and your loved ones come to terms with what’s ahead.
Questions to ask at stage 2:
- What emotional support is available?
- Can I join a support group?
- How will my family be supported?
You may be offered counselling, access to peer support, or therapies like massage or music to ease stress. Your care team can also help with sensitive conversations about your wishes for the future.
Stage 3: Enacting the care plan
This stage focuses on practical support to help you stay comfortable, safe, and as independent as possible — particularly if you’re receiving care at home.
Questions to ask at stage 3:
- Is there a plan if my symptoms change or get worse?
- What are my treatment options and their side effects?
- How can I make the most of my daily life?
Your palliative care team may arrange support from visiting carers or community nurses and help you access equipment like adjustable beds, grab rails, oxygen cylinders, or nebulisers.
If your home needs adapting, your local council may cover the cost of minor modifications under £1,000, regardless of your income. For more significant changes, such as installing walk-in showers, stairlifts, or widened doorways, you may be eligible for a Disabled Facilities Grant of up to:
- £30,000 in England
- £36,000 in Wales
- £25,000 in Northern Ireland.
These changes aim to make your daily life easier, so you can continue to live well at home for as long as possible.

Stage 4: End-of-life care begins
Stage 4 is when end-of-life care begins. The focus shifts to making you as comfortable as possible in the final phase of life, while also offering emotional and spiritual support for you and your loved ones.
Questions to ask at stage 4:
- What decisions still need to be made?
- What is a living will, and how do I create one?
- What can I expect in the final stages of my life?
Your palliative care team will work with you to plan more permanent late-stage care based on your wishes. This may involve moving into a hospice – a specialist centre offering symptom management, emotional support, and respite for families – or remaining at home with a live-in carer who understands your condition. Hospices are free of charge but typically require a referral from your GP.
If you haven’t already, this is also the time to put key decisions in place, such as creating a living will or confirming your advanced care preferences. Your healthcare team and social worker can guide you through these choices, ensuring your care reflects what matters most to you.
Stage 5: Supporting family and loved ones
This final stage of palliative care focuses on offering bereavement support to family members, friends, and carers — helping them navigate grief and begin to heal. Support is usually offered for up to 12 months, but the exact duration and type of help can vary depending on individual needs.
Questions to ask at stage 5:
- Will family members be told when the end is near?
- What support is available to family members?
- How do family members go about arranging a funeral?
Everyone processes grief differently, so your palliative care team will work to ensure support is tailored to your family — whether that’s counselling, group therapy, spiritual guidance, or practical advice. Services like Cruse Bereavement Support offer free grief counselling via phone or video call, and your GP can refer your family to local mental health services if needed.
When does palliative care begin?
There’s no definite point where palliative care should begin, however it’s generally considered that the earlier you seek support the better. Ultimately, it comes down to when you’re ready, or when you need additional support to manage a chronic illness.
While every illness is different, life-limiting conditions often share common symptoms such as fatigue, loss of appetite, mental health challenges, and pain. Having the support of professionals with the right palliative care skills can help you find physical and emotional comfort, so that you can focus on spending meaningful time with your loved ones.

Meeting your palliative care needs
Because palliative care focuses on you as a ‘whole’, and doesn’t only address physical symptoms, you’ll likely receive support from a variety of health and social care professionals, sometimes referred to as an interdisciplinary team.
It’s important to remember that the professionals providing your care should reflect and support your wishes, so don’t be afraid to speak up about what’s most important to you, and the kind of support you want.
Your palliative care team can include:
- Doctors – Your GP will be central to your palliative care, and will work with other specialist doctors and therapists to keep you comfortable and help you get the most out of your life.
- Nurses – If you’re receiving ongoing treatment, this can be provided by nurses in a healthcare or hospice setting, or at home via district and community nurses.
- Social worker – They’ll help you source practical help at home, and guide you towards key services such as family and financial support.
- Live-in or visiting carer – Professional carers can make daily life easier, providing personal care and companionship.
- A religious group – This could include helping you to attend religious or spiritual services, or visits from a faith leader to help you practice your faith at home.
- A counsellor or psychologist – They’re trained to listen and offer guidance on any fears or worries you or your family may be experiencing, and can provide ongoing support to your family.
- Charity and support groups – Organisations such as Macmillan can help direct you to additional specialist support from people who understand or have experienced your illness.