Scarlett McNally on the Importance of Keeping Active at Any Age
Tags
Living well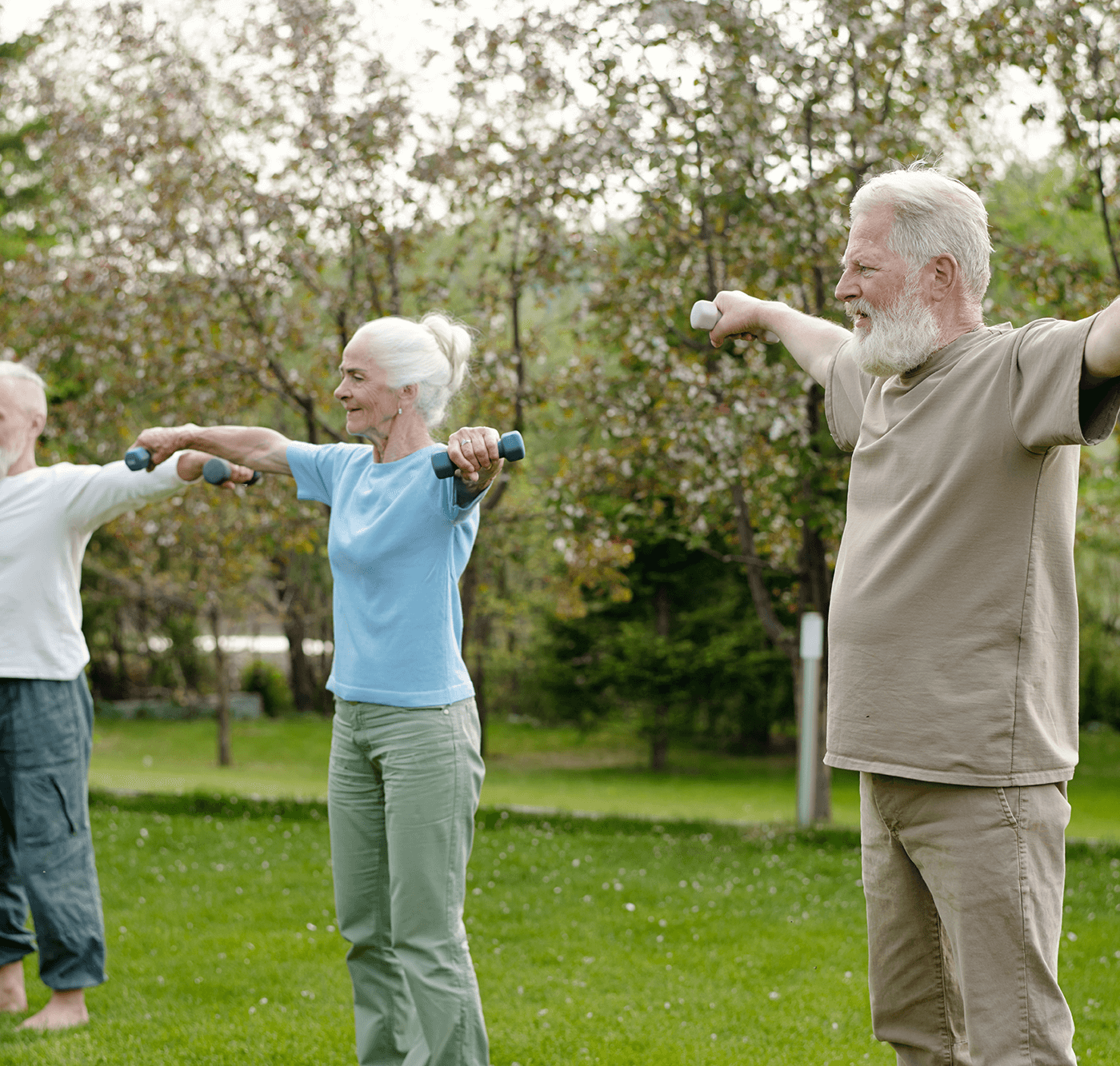

Scarlett McNally is a Consultant Orthopaedic Surgeon at Eastbourne District General Hospital, member of the Council of the Royal College of Surgeons and lead author of two hard-hitting papers on the positive impact of exercise on health. The first, “Exercise: the miracle cure and the role of the doctor in promoting it” was produced with the Academy of Medical Royal Colleges and collated data on how exercise prevents and treats diseases. The second, Focus on physical activity can help avoid unnecessary social care, was published in the British Medical Journal (BMJ) in October 2017. We talked to her about the findings of these papers and why exercise may be the best thing you can do for your health – at any age.
Where does your interest in the effects of exercise on health come from?
I qualified as a doctor in 1989, and at medical school, I realised that a lot of medical problems people were treating actually had large contributing factors. They were things that could potentially be improved with changes to environment or lifestyle, rather than with medication. That has been something that’s stayed with me ever since.
How people feel and their relationship to other people, what they eat and particularly what they do, is far more important to how healthy they are than the number of tablets they take.
Why did you use the word ‘miracle’ in the title of your paper The Exercise Miracle Cure?
I believe that if physical activity was a drug, it would be classed as a wonder drug, which is why I would encourage everyone to get up and be active.
The scales of improvements on health with exercise are bigger than the scale of most drugs though. People think a lot of diseases are caused by genetics, but only 20 percent are – most of the rest is due to environment, lifestyle and a little bit of luck.
Even many doctors don’t know that a person can reduce their risk of getting dementia and stroke by 30 percent each by doing exercise every day. Or reduce the risk of getting Type 2 diabetes by something like 40 percent. We’re busy thinking whether we should give people a pill to improve their memory, or a statin to improve their heart function.
And exercise is not just about using calories it’s about how your body manages stress and manages inflammation – which links to significant benefits of exercise around cancer.
Can we talk about exercise in terms of preventative medicine then?
Preventable is a difficult term because if I’m saying you could reduce your risk of dementia by 30 percent, there’s still a 70 percent chance that you might get it. But it is about making something potentially preventable.
There are two types of prevention. First, there is primary prevention – or never getting that disease. And then there is also something called secondary prevention, which is about doing something to reduce your risk of complications when you already have a condition.
So, if you have Type 2 diabetes and manage it well, you are less likely to get kidney failure, have infected ulcers on your feet and need amputation. Exercise is very good at secondary prevention, at a scale that is better than many drugs.
How should people be using exercise to support their health then?
The improvements in health I am talking about are based on guidelines from the Chief Medical Officer of 150 minutes’ exercise per week, or around 20 minutes a day. This means brisk exercise, so anything that gets you a bit out of breath – not an amble. So if you’re going for a brisk walk, cycling, swimming or jogging, those are great.
Our default setting as humans is sitting down, so you have to force yourself to be active. The World Health Organisation made suggestions for how to get the population more active, and one was that you have an opportunity to use the stairs, then use the stairs, because that’s really good for muscle building.
The guideline of 150 minutes a week also recommends doing something for strength-building twice a week and to improve balance. This makes a huge difference to the number of older people who fall every year.
You can improve their balance and their strength so that they’re less likely to fall – and also when they fall they’re less likely to break a bone as exercise improves bone density. It doesn’t need to be weight-bearing; indeed, I contributed to a report on swimming last year showing excellent improvements.
Fractures are incredibly common in the UK – at 65 years old, you’ve got a 20 percent chance of a hip fracture as a Caucasian woman, but about half of those that happen would have been preventable with exercise.
We need to challenge the idea that old people should rest. People need to keep active however old they are.
At 65 years old, you’ve got a 20 percent chance of a hip fracture as a Caucasian woman, but about half of those that happen would have been preventable with exercise.
Scarlett McNally
Challenging the idea that old people should rest is a controversial idea – why is it important to do so?
There is the idea in society that older people have worked hard in their lives, and being able to rest is almost a respectful thing. But actually, it’s doing them a disservice, because it really is a case of ‘use it or lose it’.
The big thing about the article in the BMJ was trying to separate out what is normal ageing, things that are common to all of us. And we find that actually, the physical decline isn’t nearly as bad as we think. Most of the physical decline that we see is because people haven’t been using their muscles.
If you’re over 60, is it too late to take up exercise?
Absolutely not. Two-thirds of adults over the age of 65 do not do enough exercise.
One of the things we found in our paper is that people who started on an exercise programme improved their fitness quite rapidly, and in fact, the people who do least have the most gain.
Just going for a walk around the block every day made a much bigger difference to those who had previously done nothing, than somebody moving from doing 15 to 20 minutes of exercise a day. Start where you are – every little bit counts.
Probably the biggest issue is around fitting exercise into a schedule. It’s important to find ways to do that. One of the best things can be something like getting a dog – people who have a dog are far more likely to go out for a walk when they don’t really feel like it.
Families can also unwittingly contribute to disabling older people’s activity. You take mum out for Sunday lunch, for example, and drive to a gastropub. You park in disabled parking because you’ve got your blue badge, and then you get a wheelchair, or you hobble a few steps, sit down, eat, and then hobble back to the car and drive home, and sit on the sofa and talk about it. We need to break this idea. It is better to go for a family walk.
How can doctors help change attitudes and raise the profile of exercise?
One of the things we’re doing in the health service is trying to improve education, and I’m on a working group with Public Health England about how we improve education for healthcare professionals. People just assume that exercise is just too easy as an answer.
And there are other issues: it can be hard for people who really do no exercise to get started, and a lot of doctors wait for an exercise professional, a therapist or a specialist physiotherapist, to tell their patient what to do. But actually, the message is really simple. It starts where you are, do some, do a bit more, and build up.
We mentioned a big study in Exercise: The Miracle Cure, that showed a large number of doctors hadn’t discussed people’s weight, for example, with patients who were obese, because they were embarrassed to.
As doctors, we’ve had so much pressure to take the patient’s point of view, and some of the initiatives are really good around listening to a patient’s agenda and shared care. However, some doctors take that to mean you can’t argue with your patient; you’ve got to listen to them in an equal dialogue.
As a surgeon, you either operate or you don’t. You’re faced with an issue at that time, and you fix that issue. I would find it difficult to be a GP because you have to keep seeing many patients again and again for the same condition, and think: “If only they stopped smoking,” or, “If only they took my advice last time and adjusted their nutrition”.
There’s a bit of me that wants to go back to the paternalistic “me doctor, you patient – I’ve seen this before, and this is what you really, really have to do” model.
Is health purely an individual decision, or does it have a social impact as well?
According to the National Audit Office, the total cost of social care in the UK for over 65s is £100bn, similar to the amount the UK spends on the NHS.
People have the idea that the NHS is there, it’s free, and it will fix you. And we do. The things we fix we are amazing at – some of the healthcare and interventions are life-changing, and we’re privileged to be a part of that.
But actually 70 percent of NHS spending is on chronic – or long-term – conditions, or most of which have a strong preventable element – and nutrition and exercise would greatly improve them.
Sometimes legislation is also needed to change things. In my career, I’ve seen far fewer horrible road traffic collisions, because we have seatbelts and less drink driving now. A little bit of legislation helps to change the culture and what’s normal about what you do.
We definitely need to raise the profile of the benefits of exercise, because we cannot afford to stay as we are. It’s getting worse year on year.
We can jiggle around with who pays for what, what the cap on care funding is and how much of your house has to go on care, but actually if we could reduce the total amount that social care costs people, that would be fantastic.
This interview was part of a series brought to you by Elder. Whether you are looking for live-in care in London or require assistance in another part of the country, Elder will ensure that all of your care needs are taken care of.
Further Information
Listen in to Mrs McNally, FRCS HERE.
Swim England’s response to the Health and Wellbeing Benefits of Swimming Report__:
http://www.swimming.org/library/documents/2570/download
http://www.swimming.org/justswim/love-swimming/health-benefits/
Or read more about her work visit her website HERE.
To follow Mrs McNally, FRCS on Twitter click HERE.
Read more care guides

The Elder care jargon buster – 49 care terms and their meaning
Like every sector, social care has a lot of its own terminology which can be difficult to get your head around, especially if you’re facing

Mobility aids for the elderly to improve daily living
Mobility aids for the elderly to improve daily living As we age, our balance can often become compromised, leading to slips, trips and falls. While

Social groups and activities for older people – how to make new friends over 60
How social connections keep elderly people healthy Losing friends and family members is, unfortunately, a natural part of later life. But it can be detrimental

What is a carers assessment?
Caring for an elderly relative is not always easy, particularly if you have a job and a home of your own to run. The carers

Dealing with a loss of appetite in older adults
Dealing with a loss of appetite in older adults Several factors, such as physical and mental conditions, medications, and vitamin or mineral deficiencies, can influence

Caring for sleep problems in elderly
Caring for sleep problems in elderly Changes in sleeping patterns are frequent in older people, and you may notice that it progressively gets worse over